March 14, 2024 – Actress Olivia Munn's candid revelations on Instagram about her aggressive breast cancer – a surprising discovery after a “clean” mammogram and negative genetic tests – was a poignant mixture of details about her cancer and a cautionary tale for ladies.
Munn revealed her 10-month battle with breast cancer, which resulted in 4 surgeries and a double mastectomy, earlier this week and used the social media page to encourage women to coach themselves concerning the disease and the importance of appropriate screening tests.
Munn's experience reveals some truths that ladies may not know: Most women develop breast cancer not have a genetic predisposition. Mammograms don’t detect every kind of cancer. An individual risk assessment – the Munns OB/GYN advisable by the doctor – may indicate the necessity for added tests to seek out tumors missed by mammography.
Olivia Munn revealed this week that she has been treated for breast cancer and has had 4 surgeries.
Munn, 43, is understood for her work on The Daily Show with Jon Stewartas economist Sloan Sabbith in HBO's political drama The newsroom, and movies including Magic Mikewrote intimately on Instagram about checking out she had an aggressive type of cancer often known as luminal B cancer, despite the fact that she had a standard mammogram and got here back negative on a genetic test that she said checked for 90 different cancer genes.
Her doctor performed a person risk assessment and determined that Munn's lifetime risk was 37%, which was considered very high. He referred her for more comprehensive tests, which revealed cancer in each breasts.
Munn said in a series of Instagram posts that she initially kept her diagnosis a secret, explaining, “I had to catch my breath and get through some of the most difficult phases before I could share it.” She praises her OB-GYN Thais Aliabadi, who has decided to calculate the chance rating. “The fact that she did it saved my life,” Munn wrote.
Munn's fighting spirit and positive attitude are evident. “I’m lucky,” she posted. “We caught it in time so I had options.” She praised the efforts of John Mulaney, her partner with whom she has a two-year-old son. He researched treatments and medications and posted pictures at her son's bedside.
Munn thanked her physicians and other staff at Cedars-Sinai Medical Center in Los Angeles and Providence Saint John's Health Center in Santa Monica, including her surgical oncologist Armando Giuliano, MD, her reconstructive surgeon Jay Orringer, MD, and her oncologist Monica Mita, MD and Aliabadi.
A spokeswoman for Munn said the actress just isn’t currently giving interviews. Spokespeople for Cedars-Sinai declined to comment on Munn's case.
Genetics and breast cancer
“Most people who get breast cancer do not have an inherited genetic mutation,” said Dr. Nathalie Johnson, medical director of Legacy Health Systems Cancer Institute and Legacy Breast Health Centers in Portland, OR, who was not involved in Munn's treatment.
“Only 5 to 10 % of people that develop breast cancer have a gene that tests positive,” agreed Joanne Mortimer, MD, director of the Women's Cancers Program and medical oncologist at City of Hope in Duarte, California. Mortimer was also not involved in Munn's care and spoke generally about treating breast cancer in cases much like Munn's.
Cancer subtypes
Luminal breast cancer has its origins inthe lumen or inner lining of the milk ducts. Both Luminal A and Luminal B require estrogen to grow, Johnson said. Luminal A has a greater prognosis and is less complicated to treat. Luminal B has a worse prognosis, she said, and it is typically called B for “poor.”
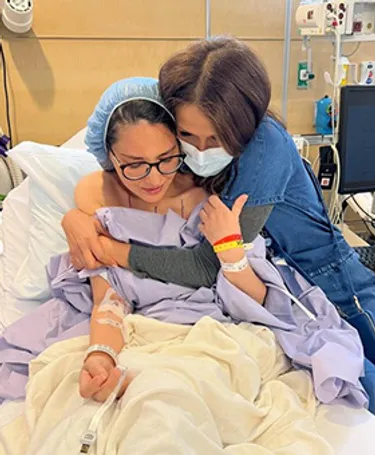
Munn is hugged by her gynecologist Thaïs Aliabadi.
Luminal B “requires chemotherapy and if it recurs; it's just more difficult. It no longer responds to endocrine therapy or estrogen blockers, so we have to resort to other therapies.”
Genomic testing helps doctors determine whether the luminal tumors are A or B forms, she said. The prognosis for luminal B cancers can still be good, Johnson said.
Beyond mammograms
“Mammograms are not perfect,” Johnson said. Cancers in breasts with dense tissue, specifically, may be missed during screening since the cancers aren’t as visible on imaging.
density refers back to the amount of fibrous and glandular tissue within the breast in comparison with fatty tissue. According to the CDC, about half of ladies age 40 and older have dense breasts. The mammogram report may contain details about whether breast density is high or low.
If the breasts are dense, an ultrasound or breast MRI can be good complementary tests, Johnson said.
Even though some cancers are missed by mammograms, Johnson urges women to get the advisable tests. The U.S. Preventive Services Task Force, In its draft suggestion, calls for mammograms to start from the age of 40 and to be repeated every two years.
Even if mammogram results show no evidence of cancer, if a girl feels anything unusual in her breasts, it's time to return to the doctor and ask for further testing, Johnson said.
An MRI is commonly performed on women at Munn's young age, Mortimer said, in the event that they are known to have dense breasts or have a family history, as each are known to extend the chance of breast cancer. “For someone with a family history, we alternate MRIs with mammograms to increase the chances of detection,” she said.
Individual assessments
In her Instagram posts, Munn praises her gynecologist for suggesting an individualized risk assessment. “DR. [Thais] Aliabadi took into account factors such as my age, my family history of breast cancer and the fact that I had my first child after I turned 30,” Munn wrote on Instagram. “She determined my risk of life was 37%.”
This result prompted the doctor to refer Munn for an MRI after which an ultrasound and biopsy. “The biopsy revealed that I had Luminal B cancer in both breasts,” Munn wrote. “Luminal B is an aggressive, rapidly developing cancer.” Thirty days later, Munn had a double mastectomy.
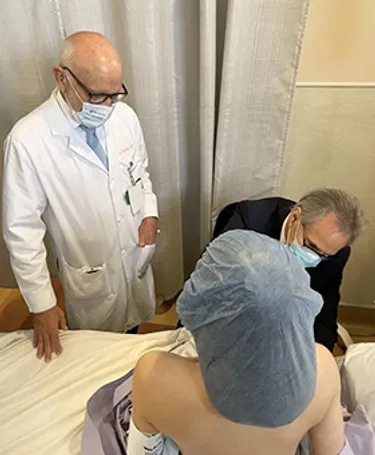
Munn is examined by two of her doctors, Armando E. Giuliano, MD, left, and Jay Orringer, MD.
Such a risk assessment is on the National Cancer Institute website. Considered history of breast cancer, previous chest radiation, genetic mutations, age, race, ethnicity, history of breast biopsy with a benign diagnosis, age at first menstrual period, age at birth of first child (over 30). increases the chance) and first-degree relatives (your parents, siblings or child) with breast cancer.
This predicts a 5-year and lifelong risk of developing breast cancer, comparing the patient's risk to the typical risk of the population.
For example, a 43-year-old white woman with no history of breast cancer or prior radiation, no genetic mutations, no prior breast biopsies, first period at age 12, 30 or older at first birth, and no first-degree relatives with breast cancer has a lifetime risk of breast cancer of 13.2%, barely above the typical risk of 12.1%.
Treatment options
In addition to the form of tumor detected, aspects resembling lymph node involvement influence treatment decisions, Johnson and Mortimer said.
For a young woman with luminal B breast cancer, the standard treatment can be surgery, chemotherapy, and estrogen blocking therapy. “The luminal B prognosis is still good if you do chemotherapy in addition to endocrine therapy,” Johnson said.
Models can assess survival rates whether treatment includes chemotherapy or not, Johnson said, helping women make their very own decisions.
Mortimer called Munn's OB/GYN “pretty amazing” when he suggested the chance calculator and took motion, discovering the tumor much sooner than the following scheduled mammogram would have.














Leave a Reply